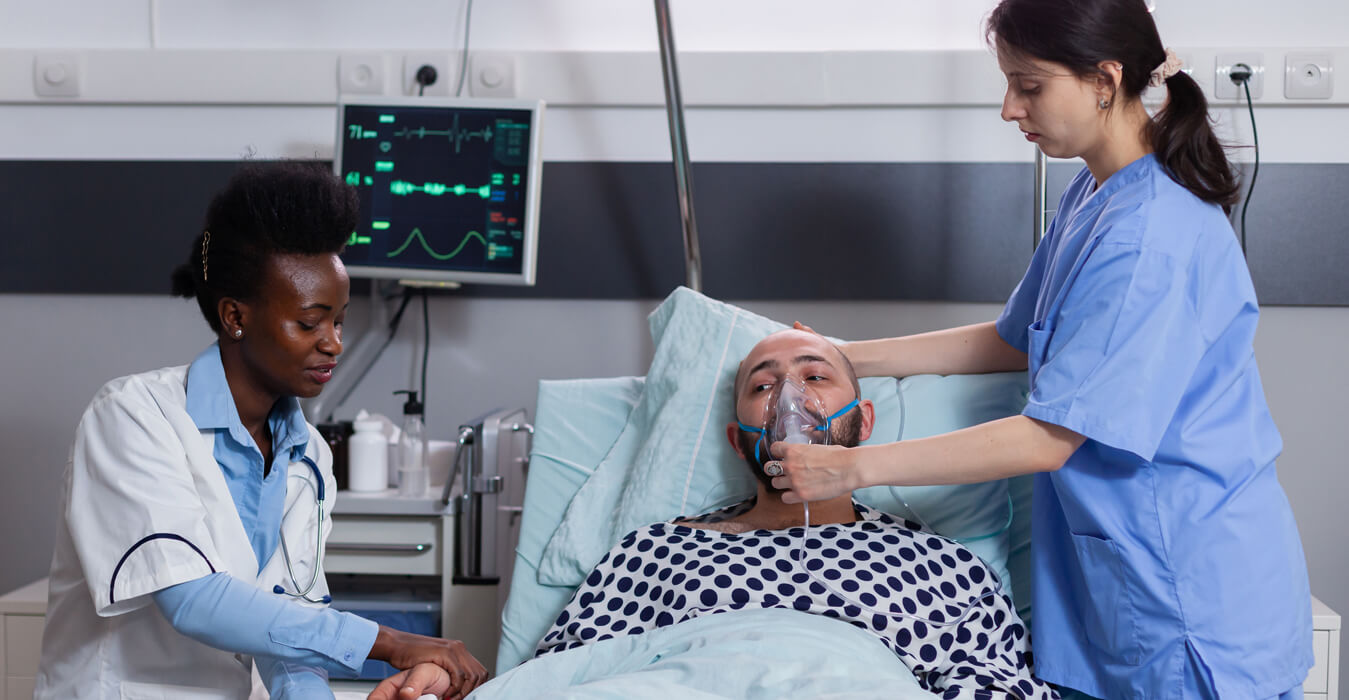
An ICU nurse’s personal story of a tormenting stay on a ventilator and how it caused her to look at her patients in a new light.
Story submitted by an ICU Nurse SkillGigger
I have been a nurse for 10 years, but in the winter of 2011, around Christmas, I began feeling ill. Before I knew it, I got so sick that I was disoriented, not realizing the perilous situation I was in. After having no contact with me for several days, my parents came to visit and realized that something was wrong with me. They quickly loaded me into the car and rushed me to the hospital.
Beginning of the ordeal
On arriving, I was forced to wait for two hours sitting in a wheelchair. At this point, I was hours away from respiratory arrest. Once I was finally triaged, I was immediately intubated and rushed off to the ICU. I can’t remember these details, of course, they’ve all been relayed to me by my family, who had accompanied me to the hospital. I was diagnosed with MRSA pneumonia in both lungs. This is only the beginning of the story.
Hallucinations and dreams
Having been an ICU nurse, as well as an ICU patient, has allowed me to voice a unique perspective on the subject. I remember awakening, for the first time, after my sedation had been reduced when my kidneys had begun to function again after suffering Acute Tubal Necrosis. The 55 lbs of water that had accumulated in my body began to be released, by way of the drug Lasix, and I was becoming stable again.
One horrible battle ahead – the ultimate reason for this story
I still had one horrible battle ahead of me, and in all honesty, this battle is the. After more than seven weeks on a ventilator, as an RN, I knew that my chances of weaning off of it were slim to none. It was my nursing knowledge of how to help wean a patient from a ventilator that enabled me to “nurse myself” and to do what I had to do to get back to the business of breathing on my own. No nurse stayed with me, even though ICU nurses only have two patients and if they have a severe case, then they have only one. There was no reason that a nurse shouldn’t have been there with me, as a cheerleader, comforter, and drillmaster, to encourage me that I could do it. Due to this reason, every day, the thought of weaning time became something to dread. Fortunately, I’m a fighter. Others may not be so fortunate to have that drive.
When the first day of weaning came, I was terrified. Part of my fear of weaning was due in significant part to the nursing care that I received. I would ring for the nurse, needing to get to the bedside chair because they had removed my catheter, but I wasn’t able, yet, to sit up in bed on my own, much less get to the bedside chair. There was more than one instance where I waited over 2 hours after calling for a nurse, but none came. I remember how I felt so humiliated when a resident came in to remove my three chest tubes. I had called for the nurse for over two hours, and finally, I couldn’t hold it anymore. I wet my bed. I rang again, and none came to change my bed. They left me in my own urine for another hour. That doctor sat down on the stool, sniffed, and looked at me in a way that I wasn’t able to comprehend. I felt like a puppy dog who had made a mistake.
Regrets and realizations as a nurse
As I began to get better and was released from the hospital to recuperate, I began to look back on my experience, as well as my career as a nurse. Had I been “That” nurse? The one who didn’t come when my patients rang. The one who left their patient to face mortifying circumstances alone. Had I judged my patients? I was relieved to come to the conclusion that I hadn’t. Had I shown them the love and compassion that drew me to the profession in the first place? I believe the answer to that question is yes.
Nurses, especially intensive care nurses, please take these words, not in a spirit of condemnation, but in the spirit of conveying the perspective of an RN turned MICU patient. If you have a patient who is heavily sedated, please understand, that hearing your calming voice on a regular basis, and orienting a patient to their situation is worth more than any other action you can perform. Be at the ready; go to them when they need you. If a patient is fearful of being taken off of the ventilator, stay put, coach them through it, and be a cheerleader. It is frightening and physically challenging to wean from the ventilator. Patients need support during this period. And always remember your patients, no matter how sedated, do perceive what is going on around them. It may be a skewed perception, but they are more aware than you know. Be the nurse who never lets them down.
So what are the critical and essential nursing skills every Intensive Care Unit (ICU) nurse must have?
- Compassion: A nurse must be drawn to caring for the sick and injured and should have empathy for the pain and suffering of patients. Listen to your patients and their families. Be accepting of family visitation.
- Communication: Make patient education a priority. Nurses must be able to communicate and collaborate effectively as they are often a patient’s advocate as well as a link between family members. Include patients and their families in bedside reports.
- Ethics: Manage patients’ pain swiftly. Regularly assess the need for invasive equipment. Nurses should need a solid commitment to humanitarian service and concern for the dignity of all patients.
- Critical Thinking: Nurses are faced with important choices on a daily basis and must be able to use critical thinking to successfully improve health care for all members of society.
- Attention to Detail: Nurses must have the ability to achieve thoroughness and accuracy when accomplishing a task. Pay attention to the details of nursing.
- Confidence: They must be confident and be able to work independently with little supervision, knowing they will get the job done.
- Adaptability: Put patient empathy at the forefront of all you do while dealing with fluctuating schedules and when required to work long hours.
- Stamina: An effective nurse needs a high energy level and a healthy lifestyle as nursing is a demanding profession that requires physical, and emotional strength, along with good mental health and psychological resilience.
- Commitment to Development: A successful nurse should be dedicated to continuing education and participation in professional organizations.
Summarizing the responsibilities of a nurse
The primary role of a nurse is to advocate and care for individuals of all ethnic origins and religious backgrounds and support them through health and illness. Registered nurses provide and coordinate patient care, educate patients and the public about various health conditions, and protect their patients and practice.
Nursing Stats in the United States
According to the U.S. Bureau of Labor Statistics, Registered Nurses encompass one of the largest segments of the workforce in the United States with over 3 million registered nurses in the country highlighting the important role a nurse plays in the healthcare industry and more specifically in caring for adults or senior citizens with disabilities or children.
How to become an RN?
Registered nurses usually take one of three education paths: a Bachelor of Science degree in nursing (BSN), an associate’s degree in nursing (ADN), or a diploma from an approved nursing program. Registered nurses must have a license from the state in which they will be working. Not to mention, specifically have at least a year or two of experience in the specialization they look forward to working as a travel registered nurse.
As a last note…
Being a patient reminded me of the essentiality of always showing empathy and compassion toward patients and their families. Intensive care nurses, please take the words in the spirit of conveying the perspective of a nurse turned ICU patient. If you have a patient who is heavily sedated, please understand, that orienting a patient to their situation is worth more than any other action you can perform. Patients need support during this period and be the nurse who never lets them down.
Curious about SkillGigs? JOIN!