Most healthcare leaders evaluating new staffing solutions start with the same assumption: “Our VMS isn’t working anymore.” But that’s not entirely true. In fact, most Vendor Management Systems (VMS) are doing exactly what they were designed to do to manage vendors efficiently.
The real issue is this:
Healthcare staffing challenges have evolved. VMS platforms haven’t.
This isn’t a failure of technology. It’s a mismatch between the problem being solved and the problem that actually exists today.
What VMS Platforms Were Built to Do
Vendor Management Systems were designed for a different era of workforce management.
Their core purpose was to:
- Centralize multiple staffing agencies
- Standardize requisition workflows
- Track spend across vendors
- Ensure compliance and documentation
For large health systems managing dozens of agencies, this created structure and visibility where none existed before. And in that context, VMS platforms still work.
The Problem: Healthcare Staffing Has Changed
Today’s staffing environment looks very different:
- Persistent nurse shortages
- Increased reliance on contingent labor
- Rising agency costs and margin pressure
- Demand for faster hiring cycles
- Need for workforce ownership and continuity
Hospitals are no longer just managing vendors.
They are trying to:
- Reduce dependency on those vendors
- Improve speed to fill
- Control labor costs
- Retain access to proven clinicians
This is where the gap begins.
The Core Limitation: VMS Manages Vendors, Not Talent
At a fundamental level, VMS platforms are designed around vendors as the center of the system. That creates several structural limitations.
1. No Talent Ownership
In a VMS model:
- Agencies own the clinician relationships
- Hospitals access talent temporarily
- Once a contract ends, the connection disappears
There is no persistent talent pipeline. Hospitals repeatedly “rent” the same talent instead of building long-term access to it.
2. Speed Is Constrained by Intermediaries
Every hire flows through multiple layers:
Hospital → VMS → Agency → Candidate
Each handoff introduces delays:
- Submission cycles
- Screening duplication
- Communication lag
Even well-run VMS programs often result in multi-week hiring timelines.
3. Cost Visibility ≠ Cost Control
VMS platforms provide reporting on spend. But they don’t fundamentally change the cost structure.
- Agency markups remain embedded
- Bill rates include layered margins
- Negotiation happens indirectly
Hospitals gain visibility, but not true pricing power.
4. Reactive Instead of Proactive Staffing
VMS workflows are triggered by open requisitions. This means:
- Talent sourcing starts after demand appears
- There is no “always-on” candidate pipeline
- Staffing becomes reactive by design
In a volatile environment, reactive staffing creates instability.
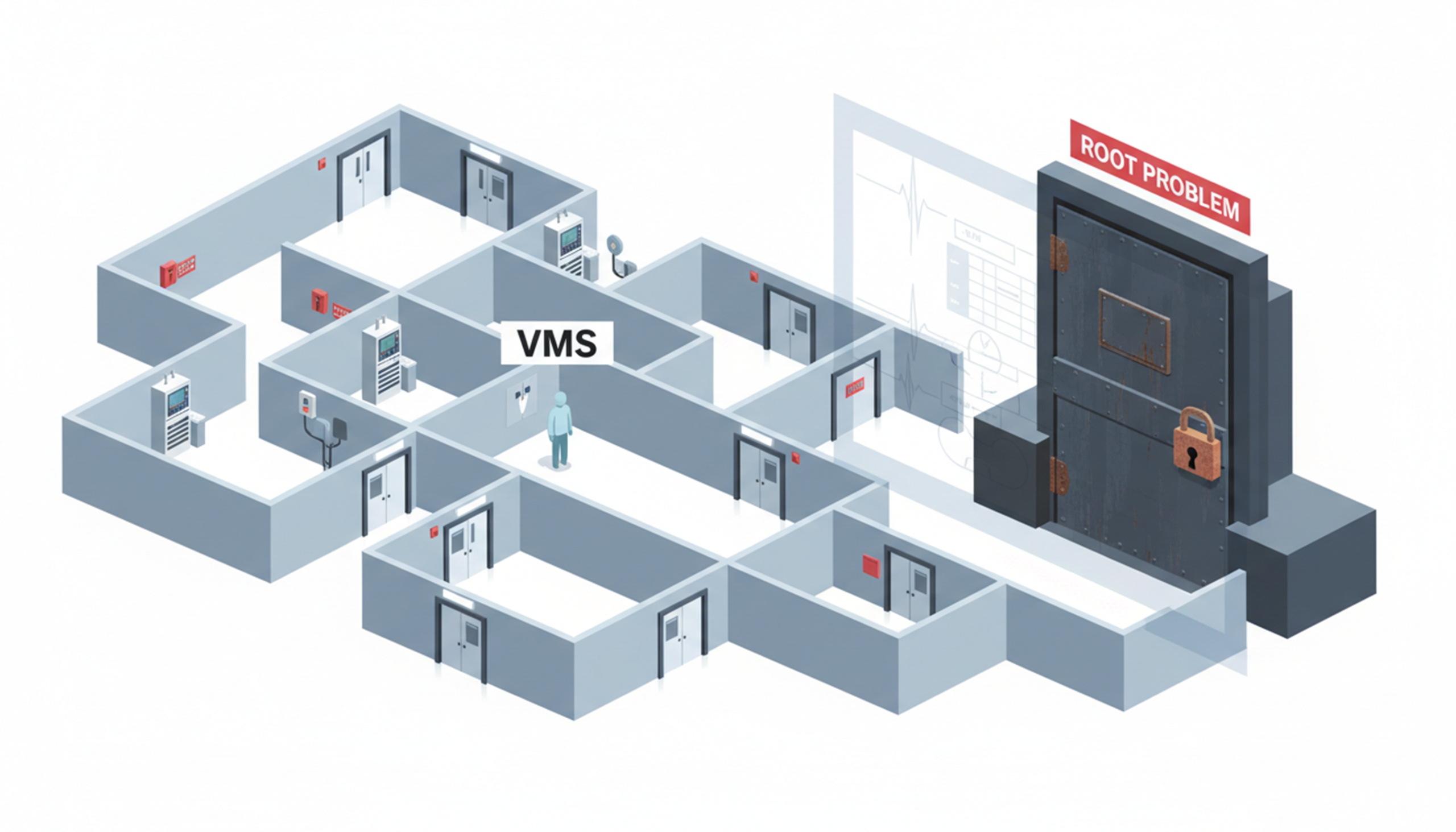
The Shift From Vendor Management to Workforce Ownership
Healthcare organizations are beginning to rethink their workforce technology strategy. Instead of optimizing vendor performance, they are asking:
“What if we owned the talent pipeline instead?”
This is where the concept of a Contingent Talent Marketplace (CTM) comes in.
How a Talent Marketplace Solves the Right Problem
A talent marketplace doesn’t replace VMS capabilities.
It shifts the focus from managing vendors → managing talent directly.
Direct Talent Access
Hospitals connect directly with:
- Nurses
- Allied health professionals
- Locum tenens clinicians
No dependency on agency-controlled pipelines.
Persistent Talent Pools
Instead of losing candidates after each assignment:
- Clinicians remain in the system
- Performance history is tracked
- Top performers are easily redeployed
This creates a living workforce ecosystem, not a transactional hiring cycle.
Faster Hiring Through Elimination of Layers
By removing intermediaries:
- Candidate discovery accelerates
- Communication becomes direct
- Hiring decisions happen faster
What previously took weeks can often happen in days.
Transparent Market-Driven Pricing
Talent marketplaces introduce:
- Direct rate visibility
- Competitive bidding environments
- Clear understanding of market value
This shifts pricing control back to the healthcare organization.
This Isn’t Replacement, It’s Evolution
It’s important to clarify:
A talent marketplace is not an attack on VMS. It’s the next layer of maturity.
In many organizations, the transition looks like this:
- VMS continues to manage vendor relationships
- Marketplace becomes the primary sourcing channel
- Agencies are used only for niche or overflow demand
This hybrid model allows healthcare systems to:
- Reduce agency dependency
- Improve hiring speed
- Build long-term workforce stability
Why MSP-Driven Models Are Feeling the Pressure
Managed Service Provider (MSP) programs built on top of VMS platforms face similar limitations:
- Focus on vendor consolidation, not talent ownership
- Incentives tied to supplier performance, not cost reduction
- Limited flexibility in rapidly changing staffing environments
As staffing becomes more strategic, these models can feel restrictive rather than enabling.
What This Means for Healthcare Leaders
If your organization is experiencing:
- Long time-to-fill cycles
- Rising contingent labor costs
- Limited access to returning clinicians
- Heavy agency dependency
The issue may not be execution.
It may be architecture. Your current system is optimized for managing vendors, not for building a modern, flexible clinical workforce.
The Bottom Line
Vendor Management Systems solved an important problem:
How do we manage multiple staffing agencies efficiently?
But today’s question is different:
How do we reduce reliance on agencies altogether while improving speed, cost, and quality?
That requires a different approach. Not a better VMS. A better model.
Evaluate Your Workforce Strategy
If you’re currently operating within a VMS or MSP framework, the next step isn’t to replace it overnight.
It’s to understand where it’s limiting your outcomes.





